Programs: Case Study #1 – Mylo Wells
A New Front Door to Care: How One Iowa Pharmacy Launched a Pharmacist-Led Walk-in Clinic
Practitioner: Mylo Wells, PharmD
Setting: Independent community pharmacy, Iowa
Care Model: Pharmacist-led, walk-in clinic embedded in a community pharmacy

Why This Case Matters
“We were seeing people who needed something right away, and their only option was the emergency room. They didn’t want to go there—but they didn’t have anywhere else to go.”
Like many Iowa communities, patients of Wells Hometown Drug faced familiar barriers to timely care: long waits for primary care appointments, urgent care visits for relatively minor conditions, and confusion about where to go for quick clinical needs. With Iowa’s new standard of care (SOC) framework clarifying and expanding what pharmacists can do based on their education, training and experience, Mylo Wells saw an opportunity to redesign access to care—right at the pharmacy counter.
Rather than adding one new service at a time, Wells launched a pharmacist-led walk-in clinic designed to function as a true front door to care for common, acute needs.
The Vision: Pharmacists Practicing at the Top of Their Education, Training, Experience
“My goal was to go to the highest level that we could under the new law, because this is exactly what it was meant for—helping with provider shortages in rural areas like ours.”
Wells’ goal was straightforward but ambitious: create a care model where patients could walk in, be clinically assessed by a pharmacist, and receive timely treatment—without unnecessary referrals or delays.
Under the SOC framework, Wells and his staff focus on what they are trained to do:
Assess patients using history collection and clinical judgment
Determine whether the condition falls within the pharmacist’s scope of practice, education, training, and experience
Initiate, modify, or discontinue therapy when appropriate
Refer to another provider when the patient’s needs exceed pharmacy-based care
The result was a clinic model grounded not in a list of rigid protocols, but in professional accountability and patient-centered decision making.

From Concept to Clinic: Implementation in Practice
“We really tried to be aggressive with what we could do—while still staying within what we felt comfortable doing as providers.”
1. Designing the Workflow
The clinic was intentionally designed as walk-in, removing appointment barriers. Patients are first screened to ensure their concern is appropriate for pharmacist management. Clear workflows guide documentation, clinical decision making, and follow-up. New policies and procedures were developed for this new format of pharmacist-provided care. Additionally, an electronic health record system was implemented to allow for pharmacist e-prescribing, when appropriate, and enhanced clinical documentation functionality as compared to what was found in Wells’ pharmacy management software.
2. Training and Confidence
A key theme from the interview was confidence—both personal and organizational. Wells emphasized the need to ensure his staff were comfortable practicing under the new SOC model, understanding when to treat and when to refer, and documenting decisions clearly. Additional training was obtained to ensure that pharmacists are able to assess and treat a broader range of ailments. An urgent care bootcamp training was used to ensure that Wells and other walk-in clinic staff were able to support patient needs.
3. Physical Space and Visibility
The clinic space was integrated into the pharmacy, reinforcing that this is not a separate business line, but an extension of pharmacy care. Signage and staff messaging consistently communicate: “You can see the pharmacist for this.” Wells is intentional in ensuring patients can choose where to pick up any prescriptions that may result from a visit to the clinic. Implementing their EHR system allows for flexibility and adherence to Iowa’s e-prescribing law.
4. Legal and Compliance Considerations
Rather than asking, “Is there a protocol for this?” the team asked, “Is this within my education, training, and experience—and is it in the patient’s best interest?” Enhanced documentation practices were implemented to reflect clinical reasoning, not checklist compliance.
What Services Are Provided?
The walk-in clinic focuses on common, low-acuity conditions where timely access makes a meaningful difference, such as:
Minor infections
Preventive and public health-related services
Medication assessment and initiation for acute needs
Patients who present with red flags or complex conditions are referred to other providers, often with guidance on where to go next. Communication with other providers is an essential part of the clinic, whether it is a referral or to share outcomes of a patient visit.

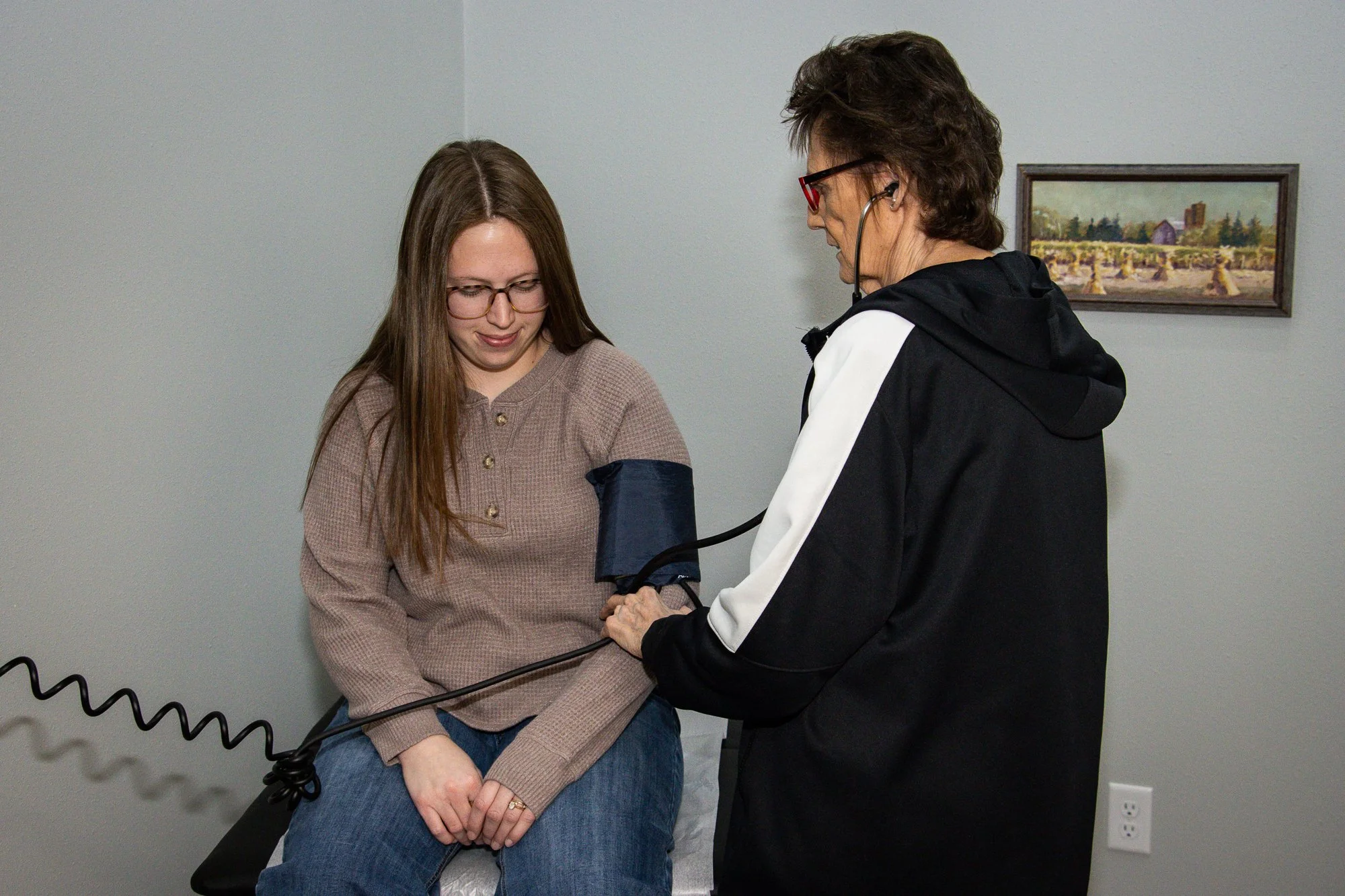
Patient Response: “I Didn’t Know a Pharmacist Could Do That.”
“Once people do it once, they’re really impressed by it. It’s just getting those people in the door the first time and becoming comfortable with seeing a pharmacist as the provider.”
One of Wells’ most consistent observations was patient surprise—followed by appreciation. Many patients initially did not realize pharmacists could assess and treat clinical conditions. After their visit, patients expressed relief at receiving same-day care without the cost or delay of having to travel farther to a traditional urgent care facility.
Over time, word of mouth became a major driver of utilization, reframing the pharmacy as a place not just to pick up medications, but to receive care.
Impact on the Pharmacy
“This has really proven that patients are willing to pay for our time.”
While patient care was the primary motivation, the clinic also delivered operational and professional benefits:
Stronger relationships with patients
Increased visibility of pharmacists as healthcare providers
Diversification of services beyond dispensing
Improved professional satisfaction for pharmacists practicing at the top of their education, training, and experience
Wells noted that the SOC framework did not increase risk—it clarified responsibility and empowered better decision making.
Key Lessons for Other Pharmacies
1. Start with patient needs, not services.
Design care around what patients actually seek treatment for.
2. Embrace professional judgment.
The SOC framework works when pharmacists leverage their education, training, and experience and document their clinical reasoning.
3. Normalize referrals.
Referring out is a strength, not a failure—it reinforces patient safety and credibility.
4. Educate patients continuously.
Every interaction is an opportunity to explain what pharmacists can do.
What This Means for Pharmacies
This case study illustrates how the standard of care framework can be operationalized in day-to-day practice—without waiting for new protocols, legislation, or payment models to be perfected.
Key takeaways for Iowa pharmacies include:
SOC enables innovation now. Pharmacists can design care models based on patient needs and their own education, training, and experience, rather than waiting for prescriptive permission.
Walk-in care is a natural extension of community pharmacy. Pharmacies are already trusted, accessible locations; SOC allows pharmacists to more easily formalize and expand the clinical care patients are already seeking.
Documentation and judgment are central. Clear clinical reasoning and appropriate referrals strengthen—not weaken—professional accountability.
Practice transformation can start small and scale. While this pharmacy launched a full walk-in clinic, the same principles apply to adding or expanding individual services under SOC.
As Iowa continues to face provider shortages, especially in rural and underserved areas, pharmacist-led care models like Wells Hometown Clinic demonstrate how pharmacies can play a critical role in improving access while advancing the profession.


Looking Ahead
This pharmacist-led walk-in clinic demonstrates how Iowa’s standard of care framework can move from regulation to real world impact. By reimagining the pharmacy as a site of first contact care, this model offers a scalable example for improving access, efficiency, and a positive patient experience across the state.
Disclaimer: This case study is based on interviews with Mylo Wells and reflects real world implementation of Iowa’s standard of care regulatory framework.
